
The patients filled out the questionnaires before and 1, 3, 6, 9, and 12 months after completing radiotherapy for the first year, and at 6-month intervals for the following years. The former includes a global health status scale, five functional scales, and nine symptom scales, and the latter comprises 18 symptom scales. The European Organization for Research and Treatment of Cancer (EORTC) Quality of Life Questionnaire (QLQ-C30) and head and neck cancer module (QLQ-H&N35) were used for HRQOL assessments. The eyes, lens, parotid glands, submandibular glands, oral cavity, lips, mandible, larynx, and brain were spared as much as possible while delivering acceptable PTV coverage. 
The maximum dosages of spinal canal planning organ at risk volume (PRV), brainstem PRV, and optic nerve PRV were restricted to 50 Gy, 54 Gy, and 50 Gy, respectively. The highest priority was to deliver the prescription dose to > 95% of the PTVs. One patient stopped radiotherapy at 58 Gy in 29 fractions because of febrile neutropenia. PTV1 was treated with 40 Gy in 20 daily fractions and PTV2 with 60 or 66 Gy in 30 or 33 daily fractions with a two-step technique. The PTV2 was defined as the boost target volume and included the primary tumor and lymph nodes known to contain metastases with the same setup margin. 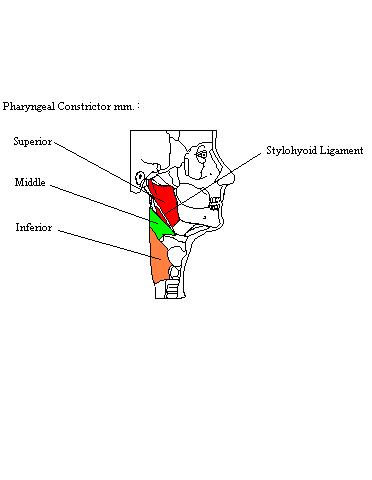
The PTV1 was defined as the initial target volume and included the primary tumor, lymph nodes known to contain metastases, and bilateral neck node levels considered at risk of microscopic disease with a 5-mm setup margin in all directions. All patients were immobilized with a face mask during their planning computed tomography acquisition of 1.25 mm slice thickness and all treatment sessions. Radiotherapy was delivered using a tomotherapy system (Accuray®, Sunnyvale, CA, USA). Regarding the parotid gland, the side that received the lower dose was selected for dosimetric analysis. were referred to for these OAR delineations. Organs at risk (OARs) delineated in this study were as follows: spinal canal, spinal cord, brainstem, brain, eye, optic nerve, lens, optic chiasma, mandible, parotid gland, submandibular gland, oral cavity, sublingual gland, cochlea, thyroid, pharyngeal constrictor muscle, superior pharyngeal constrictor muscle (SPC), middle pharyngeal constrictor muscle (MPC), inferior pharyngeal constrictor muscle, temporomandibular joint, larynx, trachea, esophagus, temporal lobe, brachial plexus, internal auditory canal, tympanic cavity, eustachian tube, pituitary, lip, and planning target volume (PTV) 1 and PTV2. We found that dosages to the SPC and parotid gland were associated with severe deterioration in HRQOL attributable to difficulty in HNSO and HNCO, whereas dosage to the MPC was associated with severe deterioration attributable to nausea and vomiting. Regarding “nausea and vomiting,” there was a significant difference between the two groups in the mean dosage to the middle pharyngeal constrictor muscle (MPC: 61.9 Gy vs. Regarding “trouble with social eating (HNSO)” and “coughing (HNCO),” there were significant differences between the severe-deterioration and mild-deterioration groups in mean dosages to the superior pharyngeal constrictor muscle (SPC) (HNSO: 62.5 Gy vs 54.2 Gy p = 0.00029, and HNCO: 61.5 Gy vs 54.1 Gy p = 0.0012) and parotid gland (HNSO: 24.1 Gy vs 20.5 Gy p = 0.000056, and HNCO: 24.2 Gy vs 20.3 Gy p = 0.00043). 
P < 0.0013 according to Bonferroni correction was considered to denote statistical significance. The relationships between HRQOL deteriorations and patient-related or dosimetry-related factors were evaluated. Patients were divided into “severe-deterioration” and “mild-deterioration” groups on the basis of degree of deterioration HRQOL > 6 months after completing treatment. These data concerned health-related quality of life (HRQOL) and were collected using the European Organization for Research and Treatment of Cancer Quality of Life Questionnaire (QLQ-C30) and head and neck cancer module (QLQ-H&N35). PRO data of 53 patients with head and neck cancer treated with radiotherapy were prospectively collected. The aim of this study was to explore the relationships between dosimetric parameters of organs at risk and patient-reported outcomes (PRO) after radiotherapy of patients with head and neck cancer.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
